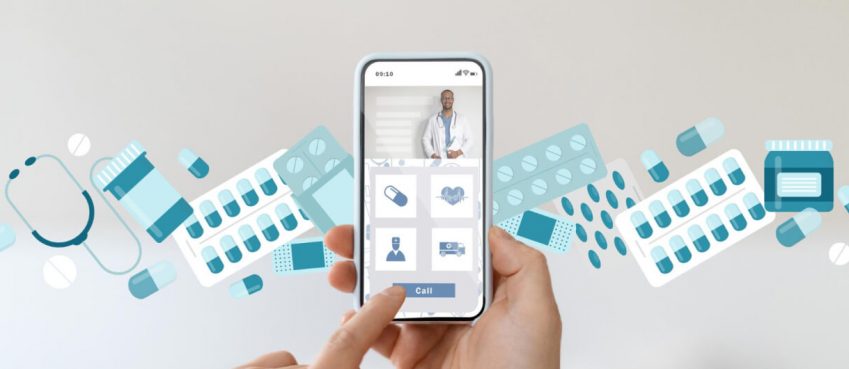
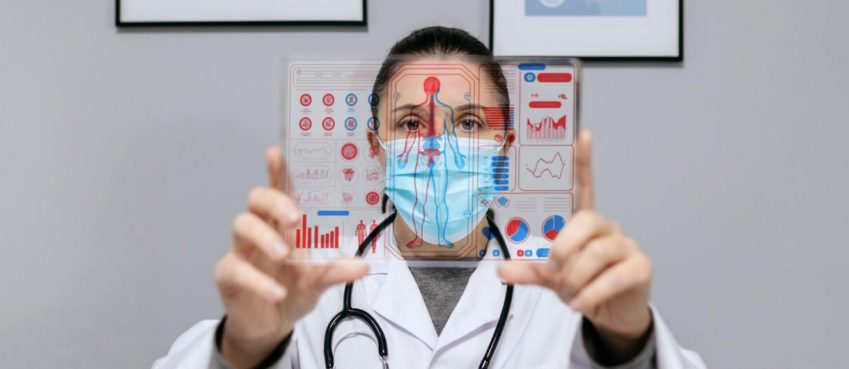
Making sure that professionals use caution in delicate treatment situations is one of the most significant advantages of Remote Patient Monitoring (RPM). The service empowers healthcare practitioners with key valuable clinical support and assistance.
However, the seamless and dependable distribution of this system raises concerns. Healthcare professionals should carefully select which patients will be watched remotely and have realistic plans in place to deal with any issues that arise.
These five most crucial actions must be completed to successfully implement Remote Patient Monitoring.
Make A Thorough Plan Before Starting
Healthcare institutions must plan Remote Patient Monitoring based on two essential perspectives. The first category is the clinical group, which defines the issues that need to be tracked and how RPM is being used to try to address them. The monitoring process should be decided by these professionals as well.
The IT team is the other group. The technological limitations that RPM plans may have gone unnoticed by many practitioners. The use of technology by physicians, particularly in patients’ homes or wearable gadgets, may also be limited. Collaboration between IT and clinical stakeholders is crucial from the start for this reason.
Before identifying the monitoring tools required to meet the objective, RPM should take into account the clinical problem the team is attempting to solve.
Also read: Walmart Pharmacy Hours & Number (Complete Guide!)Prioritize Simplicity First
Extremely complicated RPM systems must be avoided. The monitoring system should be kept as straightforward as feasible, and success should be built up gradually. Calls are one of the most efficient methods of remote monitoring.
There are straightforward methods for remote monitoring of some illnesses. One of these illnesses is heart failure since patients need to be carefully monitored. A scale for tracking weight should be available to heart failure patients. Before issues arise, the situation may be immediately handled if the weight begins to rise.
When the specialists note some alarming indications, they can immediately respond with corresponding treatment alterations, such as changing the patient’s medicine or upping the dose.
Select The Equipment That Best Suits Your Needs
Hospitals can manage RPM tools in a variety of ways. Some hospitals are in charge of the entire procedure. The equipment and installation are purchased by the institutions. They feed patient information and computerized patient records thanks to these gadgets. Some hospitals opt to use businesses to handle incident management as well as the complete RPM process.
You must recognize the areas of your decision-making process where continuity and competence are required. You can’t just let the patients figure out the problem on their own since the devices might malfunction. If you do, the patients could give up trying. Choose the obligation you want to accept or the more economical option.
Ensure Your Practices and Objectives are Clearly Stated
Why you are employing this solution is the most crucial factor in RPM communication. Patients and staff alike must have faith in what you do. If not, involvement will vanish very rapidly.
Choose the best communication strategy for each group. The training they get should be made available to patients and clinicians as well. Patients should demonstrate their ability to electronically communicate their weight. If they are unable to do so, they should continue their training. Clinicians must also identify the patient who is having issues.
Additionally, you must confirm that the software is functional before utilizing an RPM application. For instance, if you send a patient home with a scale that is connected to the internet but the patient’s home does not have internet, you must find a means to deliver this service, perhaps via a mobile device.
Use These 5 Patient-Centered Outcomes to Gauge Success
Decide on your success metrics last. The number of patients who participate in the RPM program may rise as a result of output that is process-oriented. An increase is seen from the previous month if 5,000 patients give at least one report. However, this is only a number.
On the other hand, this will be patient-focused output if individuals in an RPM pool of 500 patients notice that their monthly hospitalization rate falls from 7 to 4 percent. Even more crucial are patient-based measures. These metrics must be established at the appropriate level and must have some significance.
Top 10 News
-
01
Top 10 Deep Learning Multimodal Models & Their Uses
Tuesday August 12, 2025
-
02
10 Google AI Mode Facts That Every SEOs Should Know (And Wha...
Friday July 4, 2025
-
03
Top 10 visionOS 26 Features & Announcement (With Video)
Thursday June 12, 2025
-
04
Top 10 Veo 3 AI Video Generators in 2025 (Compared & Te...
Tuesday June 10, 2025
-
05
Top 10 AI GPUs That Can Increase Work Productivity By 30% (W...
Wednesday May 28, 2025
-
06
[10 BEST] AI Influencer Generator Apps Trending Right Now
Monday March 17, 2025
-
07
The 10 Best Companies Providing Electric Fencing For Busines...
Tuesday March 11, 2025
-
08
Top 10 Social Security Fairness Act Benefits In 2025
Wednesday March 5, 2025
-
09
Top 10 AI Infrastructure Companies In The World
Tuesday February 11, 2025
-
10
What Are Top 10 Blood Thinners To Minimize Heart Disease?
Wednesday January 22, 2025